Dear Becky –
Shortly after my father died a few years ago, you posted an open letter to him on your blog. Recently it came to me that I wanted to write a letter to you and put it there as well. At first, I was not sure what I wanted to say. I could tell you how much I loved you, and love you still, but we said this often and you know it very well. Then something occurred to me that I don’t believe I did say to you nearly enough: “Thank you.”
Thank you for sharing over 33 years of your life with me in marriage. For allowing me to spend my life with you and for our most important joint work together: Two brilliant and beautiful little girls that have now become two brilliant and beautiful young ladies.
When we married, your mom said to me, “Well, Mike, your life will never be dull.” Truer words were never spoken. Thank you for all the fun. You once gave me a card with an appropriate picture on it that was addressed to me with the words, “From a high flier to feet-on-the-ground.” I think that was one of your favorite cards that you ever gave me. And I have come to realize even more, now that you have moved on and you are flying higher than ever, how much fun you created just by being you. With Becky around, flying so high, and holding onto her balloons with one hand and onto me with the other, even a stodgy old feet-on-the-ground guy like me was dragged along into new adventures of all sorts. Thank you for that.
But maybe you needed my role as an anchor for you as well. A couple that you and I came to know as friends just this last summer commented to me after you left us that they were really impressed by how well you and I “fit” together. With people, I am not sure that opposites attract so much as that they complement each other. I know you completed me, and maybe I did the same for you. You probably would say so.
Thank you for always supporting me in virtually everything I ever suggested we should do, even when it meant totally re-arranging our life together. You almost always said yes in the little things. But you always said yes in the big things, too--always ready to go along and always totally supportive.
When I suggested that maybe we should move from Dallas, Texas, to Huntsville, Alabama, where I had a great job offer, you said this would be fine if that is what I thought we should do. You totally supported this, even though we were moving away from a place where you had good friends and quite a bit of your family. As it turned out, we ended up driving to Alabama separately. You told me later that as you were driving out of Dallas, a place where you were always very happy, the radio started playing “Let's go to Luckenbach Texas with Willie and Waylon and the boys.” At that point, as it really hit you that we were leaving, you watched the Dallas skyline receding in the rear view mirror with tears streaming down your face. But despite this attachment, you had never hesitated for a second to sign up and go happily with me to a new place. Of course, that was not the end of your story. The very next song was the group Alabama singing “My Home’s in Alabama.” And you took that as a sign that we were doing exactly the right thing. And that made you happy again. That is so Becky. So much my Becky.
Another time a few years after we moved to Alabama, you came home one night to find me lying on the picnic table in the back yard, staring at the stars. Naturally, you asked what was going on. I explained with a lot of indecision that I was considering resigning my job at the company where I had a great salary and a lot of security and a nice recent promotion. The new opportunity would be helping to cofound a tiny high risk startup company that would mean very long hours and very low money, and it could very easily fail completely (as most of them do). So this was definitely a scary proposition. Your response was almost instantaneous (and you liked to quote yourself on this for years afterwards): “Let’s go for it!” You even quit your own job and joined us as our office manager and bookkeeper. That was quite an adventure, wasn’t it?
Thank you so much for your unfaltering and enthusiastic support in these things and in every big decision we made. I don’t think most people are lucky enough to be always given the gift of that kind of absolute support and confidence from their life partner.
Your constant example taught me so much about how we ought to be living our lives, even if I seemed to be resisting some of this a lot of the time. Beside our front door up in Tennessee, I recently noticed a small colorful notice that says, “Peace to All Who Enter Here” that you placed there a long time ago. But you didn’t put that up there just because it was a cute thing to do. You really meant it. You--with your bumper sticker saying “Teach Tolerance” and another one with a big equal sign and another one that says “Namaste” on it—you believed in these things, and you lived the example that our daughters and I saw in you every day. It was not just words with you, although you certainly had the conviction to say the words, too, even when facing people who might not agree with you. Your friends, and especially all your relatives, know that! Thank you for that example.
A lot of these things, I did not appreciate as much before as I do now. I should have, but I just did not see all of them as clearly. There was often no need to push myself along some of these paths because all I had to do was to hold your hand and be dragged along to fall into the right place.
Even when you became sick, your positive attitude never failed. Your doctors all loved to see you because of your fantastic attitude and because you cheered them up. When we were doing those all day long medical visits, during our lunch break you would suggest we go to a nice restaurant. And despite everything, you would be upbeat; and we would have a great lunch and really enjoy spending the time together. That bubbly personality and virtually perpetual optimism carried all of us along and supported us all. These last few years could have been a lot harder, but you made it so much easier for everyone around you. Thank you for that gift, too.
Just about two hours before you finally left us, as you sat up in your bed, you spoke in a cheery and very casual voice to someone I could not see. You said, “OK, let’s go!” You said it twice, a minute or so apart, and you spoke in a much clearer stronger voice than any other time in those last two weeks or so. I was confused at the time, but you weren’t. Now I understand that someone had come to get you, and you were ready to go with them. And now you are on a new part of the journey without me. Temporarily without me.
From the beginning of our lives together, you and I never talked in terms of “Til death do us part.” Instead, our way of referring to our love was “Forever and always.” We both understood that this never meant there would not be other people entering our lives. Certainly when our children arrived, we loved them at least as much as we loved each other. There is always enough love. But this understanding of our permanence meant that, whatever else might be added to our lives later, our own bond would never ever be broken.
The last text message you sent to me on your phone was from the Vanderbilt Hospital in response to something I had written saying I would be back to your room later. But now I think your note had a double meaning—one that neither of us understood at the time. Your very last message said simply, “I will wait for you.” I know that you want me to get along with my life here, and I have been doing that, and I will continue to do so. I intend to keep trying new things and building new relationships and growing. And I know you would totally approve and encourage all of that. But I also know that eventually, in some way, we will be coming together again. And I know that you will be waiting for me. Thank you for that, too.
You were always unusual, so sparkling, and so very special. I always knew that about you, even before there was an “us” when you were just my sister’s pretty college roommate. But I see it even more clearly now than I ever did before, and I appreciate it even more.
Thank you so much for agreeing to share your life with me, darling, and for our two wonderful daughters.
I love you, Becky. Forever and always.
Mike
Hibiscus French 75
15 hours ago


 It was 8 hours from checking into ER before they put me in a room on the transplant floor in the hospital.
It was 8 hours from checking into ER before they put me in a room on the transplant floor in the hospital. 









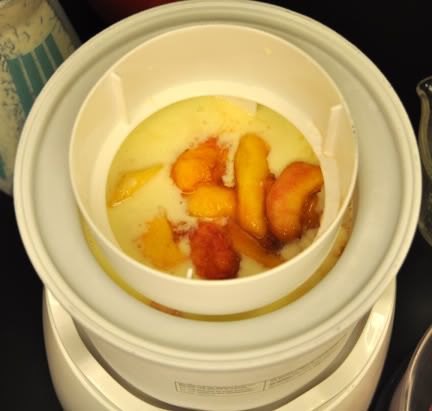





 and we got to work in the shade.
and we got to work in the shade.  During peach season my Mom and grandmother put up lots of peaches - mostly frozen and in preserves. I can remember my grandmother always put a peach kernel in every jar of her peach preserves.
During peach season my Mom and grandmother put up lots of peaches - mostly frozen and in preserves. I can remember my grandmother always put a peach kernel in every jar of her peach preserves.




















 Alabama Time
Alabama Time Paris Time
Paris Time Venice Time
Venice Time









